What’s the cause of, and the management of migraine?
Migraine is a complex neurological disorder characterised by a set of clinical signs and symptoms including moderate to severe unilateral pulsing headache attacks accompanied with nausea, vomiting, light and noise phobia, with or without aura. Unfortunately, the underlying causes of migraine include various genetic and neurobiological factors that makes their management notoriously difficult. Migraine is not a single disease but rather a syndrome that can manifest itself in a variety of conditions (Dib, 2008).
Migraine and brain energy
One of the leading hypotheses as to the causes of migraine is that it can be best described as being caused by faulty input into the brain stem from the sensory system. One of the leading trains of thought about the cause of the faulty sensory input into the brain points towards an alteration in brain energy metabolism. There is a crisis in the energy availability for the brain as well as an overload in oxidative stress in the brain that exceeds antioxidant capacity. The migraine attack itself somehow helps to restore brain energy homeostasis.
Improving mitochondrial function in the brain might be a very useful way of managing migraine symptoms. Using a high dose B2 supplement at 200mg twice a day is a very useful supplement for improving mitochondrial function as is CoQ10 300mg daily in three divided 100mg doses with food.
What are the symptoms of migraine?
It is important to recognise that headache is one of, and perhaps the most well-known, associated symptom of migraine. However, a migraine attack can often be described as having a predromal phase lasting hours to days and can include tiredness, yawning, mood change amongst other symptoms and an aura. This is followed by a headache phase of a few hours to a few days, then a postdromal phase of tiredness that can last up to 2 days.
It is well known that people who suffer from migraines may have triggers. In genetically predisposed individuals these triggers can be widely variable, however, all end up in the symptoms of migraine. Regardless of the triggers people who suffer from migraine need to modify their exposure to triggers to mitigate the severity and frequency of the symptoms but also work on and improve lifestyle factors such as improving sleep quality and quantity, exercising (which includes losing weight) eating a healthier diet with less processed foods and food chemicals, instead eating a diet rich in plant-based foods (and healthy animal products) full of vitamins, minerals and antioxidants as well as reduce and manage stress levels.

One of the most useful things being encouraged in those who suffer migraines is to keep a migraine diary. The more detail included in the diary the better, but essentially it needs to include the time you went to bed and woke up, and the quality and quantity of sleep. It should also log exercise taken, type, duration and intensity, as well as a food diary charting any foods that might trigger and scoring a daily stress level. This type of migraine diary needs to be kept for several months to be able to see a pattern in your lifestyle and what may be positively and negatively affecting symptoms.
What foods trigger migraine?
The most common foods associated with migraine include chocolate, coffee, nuts, alcohol, milk, citrus fruits and cheese. What has more recently been most strongly associated with migraines are caffeine and the food chemicals MSG and artificial sweeteners. Simply removing caffeine, alcohol and processed foods (therefore MSG and artificial sweeteners) could significantly improve the incidence and severity of migraine attacks.
Gluten sensitivity is also regarded as a trigger for a variety of neurological diseases and has been linked to headache generation. Testing for coeliac disease might be worth exploring if removing the former offending foods do not improve migraine symptoms, or you should work with a nutritional therapist regarding implementing an elimination diet.
The modern western diet is usually high in processed foods, meat and dairy and lacks vegetables, fruits and other plant-based foods rich in antioxidants. This type of diet is also pro-inflammatory, for example the western diet is high in omega six fatty acids which can convert into pro inflammatory chemicals within the body and lacking in omega-3 fatty acids which convert into anti-inflammatory chemicals within the body.
This leads to a chronic pro-inflammatory state. Working with a nutritional therapist to reduce pro inflammatory foods and increase anti-inflammatory foods as well as increasing the density of vegetables and fruits and other foods rich in vitamins, minerals and antioxidants is required.
It is also very important to control and manage blood sugar levels. As previously stated, migraine is related to an energy crisis in the brain and the brain relies purely on glucose for fuel. If that glucose supply is erratic – too much at times followed by too little may be a big trigger.
We know that fasting is a trigger for many sufferers as this reduces glucose supply to the brain. Blood sugar should be stabilised but eating healthy sources or protein and fats at every meal (including animal products) as well as low and slow releasing carbohydrates – such as plenty of brightly coloured vegetables, some fruits, nuts, seeds, beans and legumes.
Eating as much organic food as possible (or at least thoroughly washing your food) will also lower the cocktail of chemicals sprayed onto these foods. Alpha Lipoic acid helps stabilise blood sugar but is also a powerful antioxidant and mitochondrial nutrient. 300-400mg twice daily is useful in the presence of poor glucose tolerance or poor HbA1C measures.
Migraine and the female menstrual cycle
Migraines have a higher frequency in women especially after adolescence through to the menopause. One theory is the fluctuations in oestrogen can lead to migraine is genetically susceptible women. A quicker drop off of oestrogen in the late luteal phase has been noted in women suffering migraine.
Unfortunately, this is very difficult to measure. However, using phytoestrogens to mitigate the rapid decline in fluctuating oestrogen in women who suffer hormonal migraines may be useful. Speaking to your GP about how HRT may benefit you or using a supplement with greater than 60mg of soy isoflavones (genistein and daidzein) for 3 months may help.
It should also be noted that these migraines could also be linked to iron deficiency as iron deficiency anaemia can contribute to migraine. Correcting anaemia can reduce severity, duration and frequency of migraine. It’s best to have a blood test done looking at iron levels, then where necessary start with food and increase red meat consumption as a haem source of iron, then consider a supplement of 28mg a day as a glycinate form.
Manual treatment and Botox for migraines
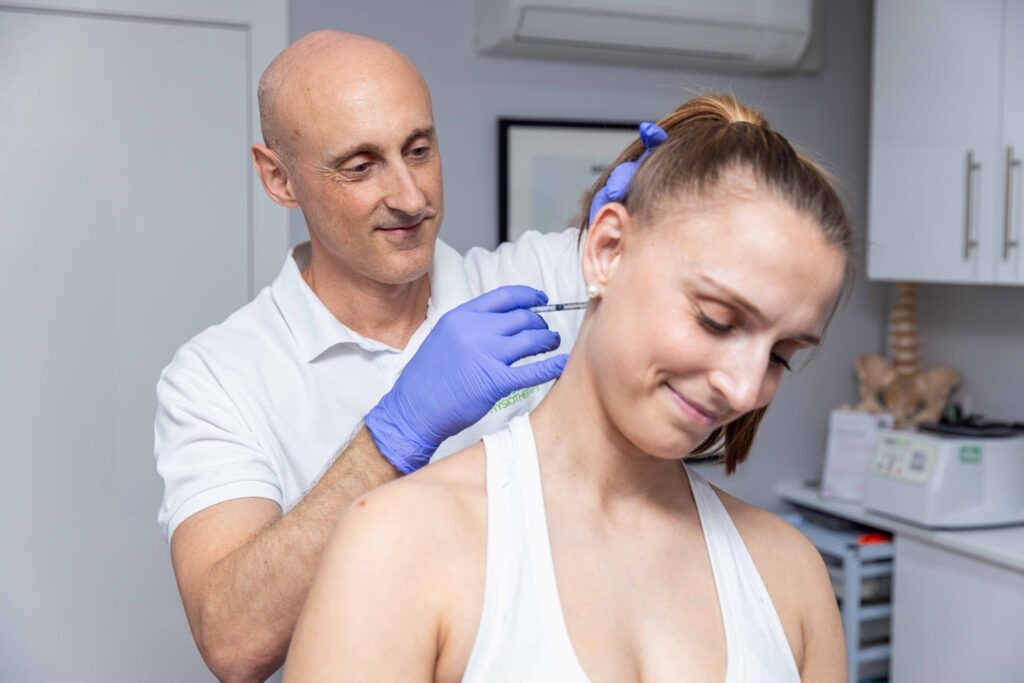
Headaches and migraine may also be mediated from the muscles of the head and neck and having treatment on these areas to mobilise the neck joints and massage or acupuncture the sore muscles can also provide relief. Botox injections into various muscles of the face, head and neck have also been used and is licensed as another form of treatment.
Are there any migraine tests and markers?
Research is being undertaken to see if there are specific tests that can be done to highlight the susceptibility to migraines and work on interventions. However, to date there is no magic test or intervention. However, beyond the individualised interventions mentioned above there are certain biomarkers that we can work with.
The first is weight and body fat. We can chart weight in kg and body fat using bio-electrical impedance or by using callipers. We can also use a tape measure to assess waist circumference and waist to hip ratio. Using this data, we can start to put together a weight management and exercise plan.
The remaining battery of tests we have relate to the points previously raised in this article. We can measure various markers in the blood that can look for oxidative stress (Glutathione, lipid peroxides, 8-OHdG, HbA1c), inflammation (CRP or omega-3 to omega-6 index), the management of blood glucose (fasting glucose, HbA1c) as well other nutrient deficiency (iron and B vitamin status).
Correcting nutritional deficiency based on this blood workup helps to personalise nutritional intervention for people with different subtypes of migraines.
Nutritional supplements and migraine
B vitamins – a simple blood test that measures homocysteine can highlight the need for B vitamins. Supplementing B vitamins may be useful in helping people with migraines. There are certain genotypes that require more B vitamins due to polymorphisms in MTHFR genes. Supplementing with a broad-spectrum form of the methylated B vitamins may be useful and should be used for at least 6 months.
Magnesium levels are often low in people through dietary intakes and the foods that contain magnesium such as fish, green veg and nuts and seeds. The dose required in migraine treatment should be 600mg per day for 3 months. The type of magnesium is also important – using magnesium citrate is very useful.
Most people are Vitamin D deficient, and deficiency is common in those that suffer from migraine. We get vitamin D from sunlight however it’s easy to take a supplement to boost levels in the body
Omega 3 should be increased in cases with those who have higher markers of inflammation (hs-CRP).
Low Zinc levels can be associated with migraine and supplementation can be helpful. A high phytate diet / vegetarian diets will usually be low in zinc. Supplement with 15mg a day.
Most nutritional interventions to mitigate migraine take months to have an effect and much like certain medication may not work for some people, however there are some nutritional analgesics that can be used to treat acute migraine.
Taking 400mg of a ginger powder product with 5% gingerols alongside analgesics might be very useful. Niacin which is a useful vasodilator may have an effect in improving blood flow in the brain. A single dose of 500mg may be useful in avoiding acute migraine during an attack.
If you suffer from migraines our headache clinic is for you. It recommended you book a Headache Assessment and Treatment session (this is a structural assessment and treatment session with a physio or osteopath) as well a Nutritional Therapy for Headaches to address many of the issues raised in the article.
References
Dib, M. (2008). Optimising prophylactic treatment of migraine: subtypes and patient matching. Therapeutics and clinical risk management. 4 (5) 1061-1078.